Kenya continues to face a significant surgical access gap, particularly in women’s health.
Maternal mortality remains approximately 355 deaths per 100,000 live births (KDHS 2022). Specialist surgical skills are unevenly distributed, with advanced procedures concentrated in urban centres.
In many facilities, open surgery remains common, leading to longer hospital stays, higher infection risk, and increased cost of care.
The Hem Practice is responding to this gap through a locally developed training model that strengthens minimally invasive surgery (MIS) skills among practicing doctors.
“This is not just training. It is a deliberate effort to make minimally invasive surgery the norm and not the exception in Kenya,” said Faith Wanjeri, Co‑Founder The Hem Practice.
The organisation today marked the graduation of Cohort 2 of its Stitch & Knot Laparoscopic Suturing Programme, an 8‑week structured skills initiative for Ob/Gyns and Registrars.
The programme is powered by the Endo Bora Pelvic Trainer, a portable simulation tool developed locally over three years to enable consistent home-based practice.
Minimally invasive surgery offers smaller incisions, shorter recovery time, reduced complications, and lower overall cost. However, equipment alone does not close the gap. Skill does.
Participants commit to a minimum of 30 minutes of daily practice using the portable trainer. Progress is measurable. Improvement is tracked. Competence is built deliberately.
Cohort 1 recorded 70pc female participation. Cohort 2 reached 80pc, reflecting The Hem Practice’s intentional focus on strengthening female surgical leadership in a traditionally male-dominated field.
“When doctors practice consistently at home level, competence increases and outcomes improve. This reduces costs and strengthens confidence in theatre,” Faith Wanjeri added.
Graduates from earlier cohorts report measurable growth. Some participants have tracked improvement from 44 pc to over 80 pc competency scores within the programme cycle. Others report significant increases in speed and precision, including completing 11 laparoscopic knots within 30 minutes.
Board Chair Dr Stephen Mwatha emphasised the broader system impact. “Training. Support. Surgical skills at home level. When these skills are shared across hospitals, minimally invasive surgery becomes mainstream. That saves lives and reduces costs at a community level.”
He noted that improved MIS capacity contributes to shorter admissions, reduced infection risk, and greater access for women who cannot afford prolonged hospital stays.
The training model is paired with service delivery initiatives such as Lap on Wheels, where surgical teams support county facilities and expand access beyond major cities.
Dr. Dennis Mureithi, who led the development of the Endo Bora Pelvic Trainer, explained that while suturing programmes exist globally, this version was modified for local realities.
“It took three years to refine. We adapted the model to fit our environment so it delivers real impact. The long-term vision is for laparoscopy to become a common skill before doctors leave medical college.”
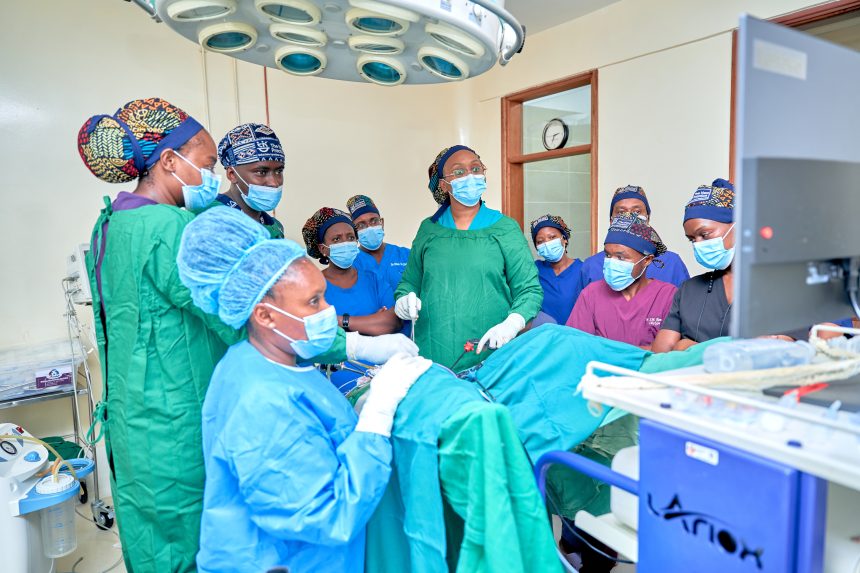
The Cohort 2 graduation concluded with a surgical camp at Maryhelp Hospital, where the 11 participants applied their skills in a live clinical setting.
As Kenya continues to confront uneven surgical access, The Hem Practice’s model positions structured simulation, disciplined repetition, and mentorship as practical solutions to strengthening women’s health outcomes across the country.